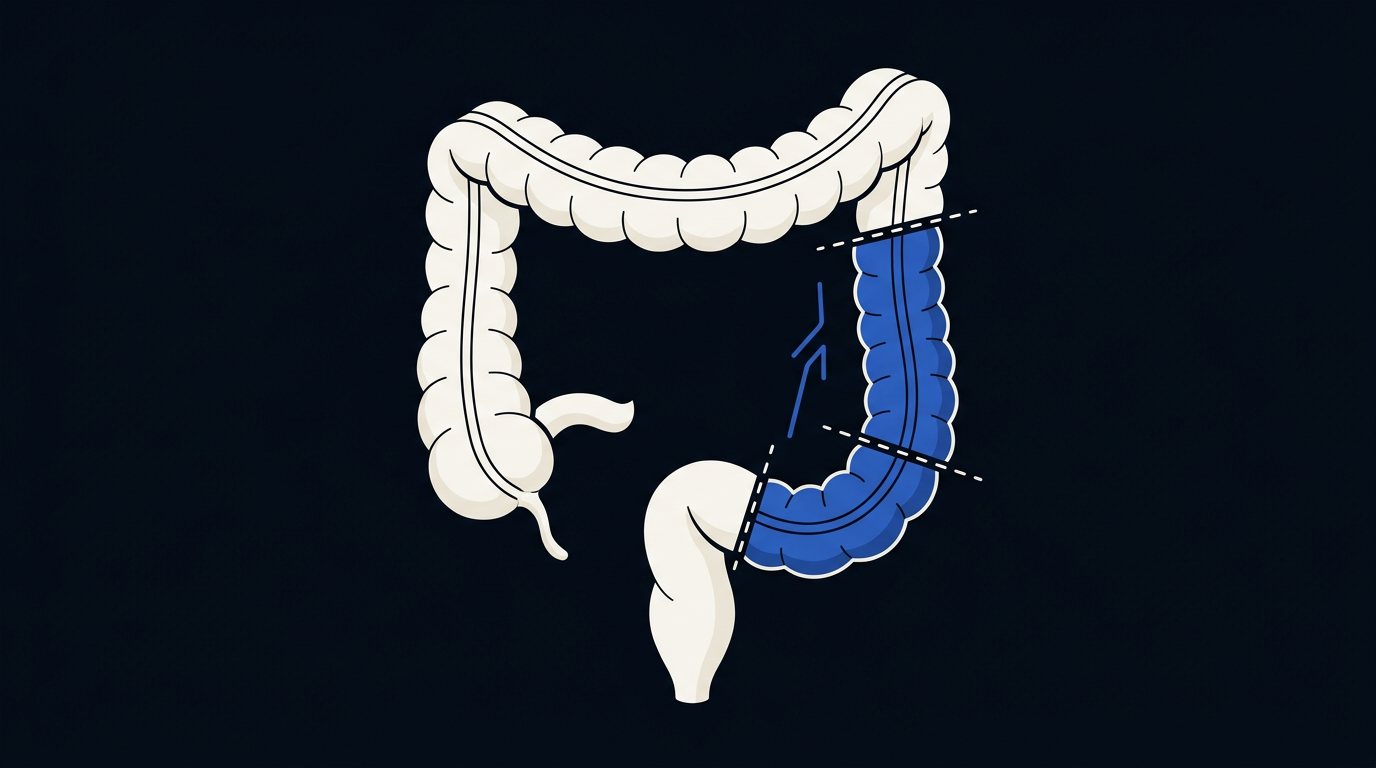
Indications
When colon surgery is recommended
Planned colon surgery is most commonly performed for colon cancer, large polyps that cannot be removed endoscopically, and complicated diverticular disease. Inflammatory bowel disease (ulcerative colitis, Crohn's) may also require surgery.
Emergency colectomy is performed for perforation, complete obstruction, uncontrolled bleeding, or toxic colitis. The urgency of the situation determines the surgical approach.
- Colon cancer or large polyps
- Complicated diverticulitis
- Bowel obstruction
- Inflammatory bowel disease complications